As a GP working in a busy inner London practice, I’m getting increasingly used to hearing the words, ‘I’ll just check my app’. Whether the consultation is about blood pressure or mental health, there seems to be an app for just about everything. But is there a market for these to be made available on prescription?
Case study: the certified contraceptive app
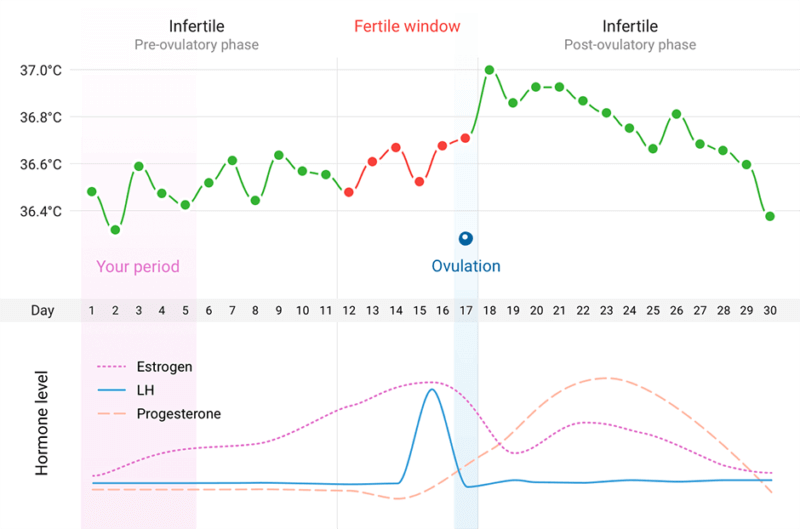
Many of you will have heard of Natural Cycles, branded as ‘the only certified contraceptive app’ it has been getting a lot of attention. For those of you who haven’t, essentially it uses a woman’s body temperature to map her menstrual cycle. It then uses this information to predict when she is ovulating, her fertility and when her next period is due (see figure 1). Clinical studies have shown that Natural Cycles is 93% effective when used as contraception.
Figure 1 – the link between body temperature, ovulation and fertility taken from the Natural Cycles Website
Working in family planning means that I am constantly being asked about the app. But I was recently taken aback when a patient who had struggled with hormonal contraception requested the app on prescription. I had to inform her that unfortunately, we are not currently able to prescribe apps on the NHS.
But this got me thinking, why not?
Cost-effectiveness
To purchase the Natural Cycles app costs individuals £39.99 per year ($79.99 in USA). In comparison, Yasmin, one of the most commonly prescribed oral contraceptive pills in the UK, costs the NHS £58.80 per year – that’s 47% more than the app. Research carried out at the Karolinska Institute in Sweden found the app to have a similar Pearl Index to the pill. So if the economics make sense, what is stopping us from prescribing?
Current health apps
App stores feature thousands of health-related apps (see figure 2). So how would clinicians decide which ones to prescribe? We can currently only prescribe weight loss pills if a patient meets a strict criteria looking at their BMI and medical history to name a few. This is to ensure that the prescription is cost-effective. One of the challenges would be to create relevant prescribing criteria for all potential health apps. This would involve multiple cost-effectiveness analyses, not an easy task!
Figure 2- Some of the health apps currently available on the App Store

Data protection
What about privacy? Huckvale et al assessed the extent to which apps which were certified as clinically safe and trustworthy by the UK NHS Health Apps Library complied with data protection principles. They found that 89% of apps transmitted information to online services and 66% sent identifying unencrypted information over the Internet. Arguably, the most important factor in the doctor-patient relationship is maintaining trust. Probably the biggest challenge, therefore, will be ensuring such apps can provide a trusted resource for patients and healthcare professionals.
The future
If an app is proven to be clinically effective then I should be able to offer it to my patients. However, this must balance with the potential repercussions. These may include the cost of such apps, and like all drugs currently being offered on the NHS, the apps must also meet the NICE cost-effectiveness threshold for prescription.
However, even more concerning are the potential privacy breaches. Perhaps blockchain technology with its encrypted digital ledger will pave the way forward in this respect. Early research has shown that blockchain could transform healthcare while maintaining patient confidentiality.
However this is still very much in the trial phases, so, for now, I will continue to apologise to my patients that apps are not currently available on prescription!





